In dermatology and skincare, diagnostic tools play a crucial role in helping doctors understand what lies beneath the surface of the skin. One such tool that has been in use for more than a century is the Wood lamp. Although it might look like a simple handheld light, it has the ability to reveal conditions that the naked eye often cannot see. For patients, understanding how a Wood lamp works and what it can detect provides reassurance when visiting a dermatologist. For medical professionals, it remains a quick, cost-effective, and non-invasive diagnostic aid.
This article explains what the Wood lamp is, how it works, and what exactly it can detect on the skin.
The Wood lamp, sometimes called a Wood’s light, was named after the American physicist Robert W. Wood, who developed it in the early 20th century. Essentially, it is a diagnostic lamp that emits ultraviolet (UV) lightin the range of about 320 to 400 nanometers. The device typically contains a filter that removes visible light, allowing mainly long-wave ultraviolet light (also called black light) to pass through.
When this UV light shines onto the skin in a darkened room, certain substances and microorganisms will fluoresce, or glow, in distinct colors. This fluorescence provides doctors with valuable clues about skin infections, pigment disorders, and other conditions.
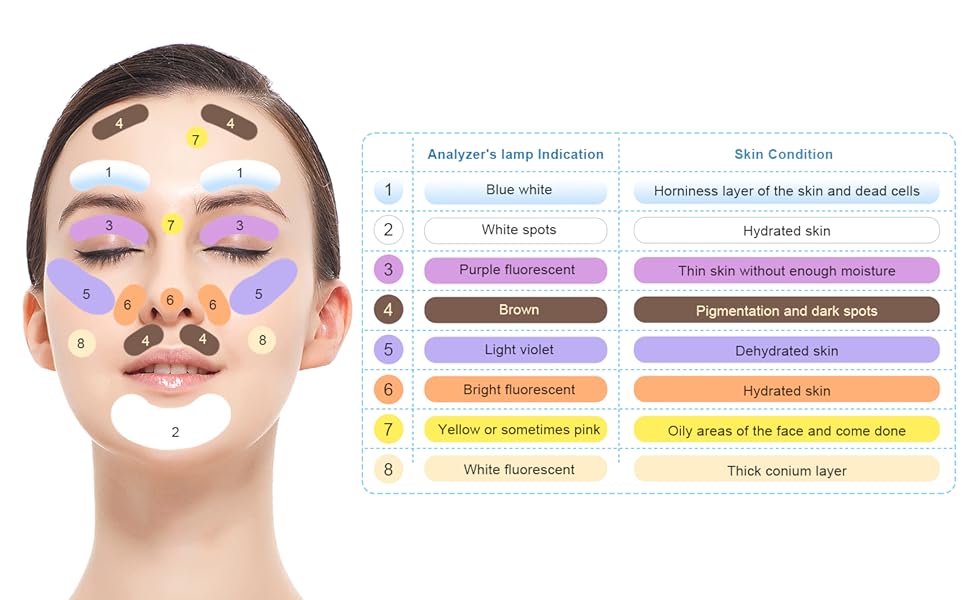
At the core of its function is fluorescence. Many materials, including some bacteria, fungi, and chemicals, absorb ultraviolet light and re-emit it at a longer wavelength, often as visible colors. Under a Wood lamp:
Normal skin usually appears a slight bluish or violet hue.
Abnormal substances or organisms show specific colors, depending on their chemical composition.
Pigmentary disorders become more defined, allowing clearer visualization of their borders.
The examination is quick, painless, and safe when performed properly. Because the Wood lamp uses long-wave UV light, the exposure is far less intense than the UV rays that cause sunburn.
The usefulness of the Wood lamp lies in its ability to highlight skin conditions that may otherwise appear subtle or invisible under regular light. Below are the most common findings:
Certain fungal species glow under the Wood lamp. For example:
Microsporuminfections of the scalp can fluoresce a bright greencolor.
Some types ofTrichophytonmay also fluoresce, though not all species do.
This makes the Wood lamp a valuable first-line tool in diagnosing tinea capitis(scalp ringworm) in children.
Some bacterial infections produce characteristic fluorescence:
Corynebacterium minutissimum, the cause of erythrasma, shows a coral-red glow.
Pseudomonasinfections may fluoresce a greenish color.
These patterns help differentiate bacterial infections from other skin rashes that look similar.
The Wood lamp is especially useful in evaluating changes in skin pigmentation.
Vitiligo: Areas of lost pigment appear as bright, chalky white patches, more noticeable than in daylight.
Melasma: The lamp can reveal whether excess pigment is in the epidermis (upper skin) or deeper dermis. Epidermal melasma appears darker and sharper under UV, guiding treatment decisions.
Post-inflammatory hyperpigmentation: Spots left after acne or injury become more distinct.
For dermatologists, this helps in assessing the extent and depth of pigmentation, leading to more accurate treatment planning.
Patients with certain forms of porphyria, a rare metabolic disorder, show pink to red fluorescenceof urine, teeth, or skin under Wood lamp examination.
In acne patients, Wood lamp may highlight skin oils and bacterial byproducts that fluoresce orange-red, helping doctors assess the degree of oiliness and bacterial colonization.
Scabies burrows sometimes become visible as grayish lines.
Changes in hydration of the skin can be detected; dry skin appears different compared to well-hydrated areas.
Some cosmetic concerns such as hidden sun damage or uneven tone can be revealed under the lamp, making it a tool in aesthetic clinics as well.
While extremely useful, the Wood lamp is not a perfect diagnostic tool. Some important points to remember:
Not all fungi or bacteria fluoresce. For example, manyTrichophytoninfections remain invisible.
Environmental factors like soaps, deodorants, or fibers may cause false fluorescence.
The examination requires a completely dark room to be effective.
It should always be used alongside other clinical evaluations and laboratory tests for confirmation.
Thus, the Wood lamp is best considered a supporting tool, not a definitive diagnostic method.
For patients, the procedure is simple and non-invasive. A dermatologist typically asks the patient to sit in a darkened room. The lamp is held a few centimeters above the skin and slowly moved across the area of concern. The exam usually takes only a few minutes.
Patients feel no pain—just the mild sensation of light shining on the skin. If the examination involves the scalp or hair, the doctor may gently part the hair to inspect the roots. The results are immediate, which can reduce patient anxiety compared to waiting for lab reports.
Even though more advanced imaging and laboratory methods exist today, the Wood lamp remains relevant because it is:
Quick and easy– requires no preparation.
Cost-effective– affordable for both clinics and patients.
Non-invasive– no skin scraping or blood test is needed.
Immediate– results can be seen on the spot.
It serves not only in hospitals but also in general clinics, dermatology offices, and even some aesthetic centers.
The Wood lamp is not restricted to disease detection. Cosmetic professionals use it to:
Identify areas of sun damage before they become visible.
Map out skin type variations for personalized skincare routines.
Demonstrate the effects of improper cleansing, where makeup or oil residues fluoresce under the light.